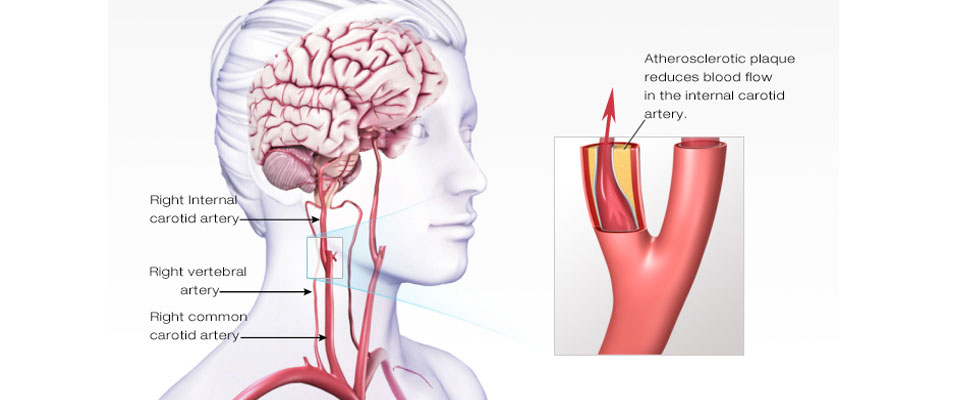
What Is Carotid Artery Disease Strokes?
The purpose of carotid surgery and stenting carotid arteries is to prevent strokes. Transient ischaemic attacks are referred to as strokes lasting less than 24 hours. There are two main types of stroke: Hemorrhagic and ischaemic. According to the worldwide data available, 80 percent of strokes are ischaemic.
There are two main types of stroke: Hemorrhagic and ischaemic. According to the worldwide data available, 80 percent of strokes are ischaemic. The embolism of diseased carotid arteries in the neck results in a high proportion of ischaemic strokes. Embolism means that a blood clot forms in one place and then breaks off and travels through the circulation to another location. The carotid arteries in the neck provide the brain and are prone to the formation of localized atheromatous plaque. On the surface of the rough plaque, small blood clots form and break off and lodge in the brain. This results in different symptoms depending on the size of the embolus and the part of the brain in which it ends.
Problems Caused By Carotid Artery Disease
Asymptomatic: CT and MRI scans often reveal evidence of several small strokes without previous symptoms. These patients may not have obvious symptoms such as mini-stoles, but they may develop impaired brain function over time, which may lead to dementia (so-called multi-infarct dementia).
Amaurosis Fugax: Small blood clots from the carotid artery may flow through the circulation to the retinal artery in the eye causing the characteristic symptom of a greying out of the vision in one eye. Patients often describe it as coming down as a curtain. Within a few minutes, the vision returns to normal.
A transient ischaemic attack (TIA) is a small stroke that takes 24 hours to resolve. Strokes resulting from blockages are the middle brain artery in the brain and paralyze the damaged artery on the opposite side. It is said that strokes lasting less than 3 weeks are transient strokes. After 3 weeks, persistent deficits are identified and the subsequent recovery can be good, moderate or poor. These clinical distinctions are important because the prognosis is related to the present symptom after carotid surgery.
How Can Carotid Artery Disease Be Tested Best?
Any patient with a carotid duplex scan should have one of the above symptoms. This determines whether the internal carotid artery is desired and, if so, the degree of stenosis. The percentage stenosis is the best predictor of the probability of a subsequent stroke currently available.
What Is The Risk Of A Serious Stroke Following A Min-Stroke?
A patient with amaurosis fugax, TIA or stroke associated with stenosis of the relevant internal carotid artery exceeding 70 percent has a high risk of severe stroke in the following three months. The correction of vascular risk factors (stop smoking, treat hypertension, initiate aspirin and statin therapy) can reduce this risk, but the correction of the underlying carotid artery disease by surgery or stenting is highly effective in reducing the risk of subsequent strokes to normal levels.
What Is An Endarterectomy Of Carotids?
Carotid endarterectomy is an operation to unblock damaged brain arteries that cause strokes if left untreated. The operation involves exposing the carotid arteries, opening the vessel and carefully removing the plaque leaving a smooth inner lining. To avoid narrowing, the artery is usually closed with a patch. During the operation, a shunt may be used to preserve the blood flow of the brain while the artery is open, but this is not always necessary. The surgery may be performed under local or general anesthetic. We usually prefer the local anesthetic technique so that the patient remains aware.
Side Effects And Problems Of Carotid Surgery
Depending on the operating surgeon and the risk factors of the patient, carotid endarterectomy has a risk of death and stroke of about 2-3 percent. This is much less than the risk of stroke or death from the untreated artery. The other major complication is damage to the area's important nerves. The most important are the hypoglossal nerve that controls the vagus nerve's tongue, mouth and branches. Some patients notice that their voice is a little hoarse or that their tongue is tedious. Fortunately, these problems are quite rare and usually temporary.
Carotid Artery Stenting
Carotid artery stenting is a relatively new way to correct carotid artery blockages for the same purpose as carotid endarterectomy to reduce the risk of stroke. The procedure is performed under local anesthetic. A fine wire and catheter are inserted into the groin into the femoral artery and passed under Xray into the neck. A balloon is inserted through the blocked artery along the wire and the balloon is inflated to open the narrowing area. After the balloon has been removed, a stent (fine metal mesh tube) is then inserted to hold the artery open. The procedure takes approximately one hour and the discharge takes 24 hours.
The problem with passing wires, catheters and balloons past a diseased artery is that it can cause debris to break and lodge in the brain causing a stroke. For this reason, most carotid artery stenters are equipped with a so-called brain protection device that is a filter to catch any debris before it can pass to the brain and cause damage. Stenting the carotid artery has the advantages of avoiding incisions and there is no risk of nerve damage in the neck. Whether the risk of stroke during carotid stenting is higher than carotid surgery is uncertain.
Asymptomatic Stenosis Of Carotid Arteries
The carotid arteries are often furred up without warning signs. The risk of stroke-causing blockages is much lower than the risk of blood clots, but they are still associated with an increased risk of stroke. There are now very good quality studies that show that even if there were no previous symptoms, the correction of carotid artery stenosis (narrowing) significantly reduces the long-term risk of fatal or disabling stroke. The benefit depends on the patient's degree of narrowing, age and gender.